What is Pompe disease?
About Pompe disease
Pompe disease is a rare genetic condition that runs in families. It is also known as acid maltase deficiency (AMD) or glycogen storage disease type 2. Pompe disease belongs to a larger group of conditions known as lysosomal storage disorders.
Pompe is a debilitating and potentially life-threatening neuromuscular disorder. Like all lysosomal storage disorders, it is lifelong and progressive, which means it can get worse over time. Symptoms can often go unrecognized or are initially misdiagnosed. However, the earlier Pompe disease is diagnosed, the sooner it can be appropriately managed.1,2
If you think you or a family member may have Pompe disease, talk to a doctor about possible next steps such as getting tested.
How common is Pompe disease and who does it affect?
Pompe disease can affect both males and females. The estimated occurrence of Pompe disease is around 1 in every 40,000 individuals.
The condition is generally classified into two types, which differ in their severity and age at onset. Late-onset Pompe disease can present at any age, usually from childhood to adulthood, whereas infantile-onset Pompe disease affects infants within the first year of life and is more severe.1
What are the signs and symptoms of Pompe disease?
Pompe disease symptoms and the age at which they present can vary from person to person. The late-onset type can present very differently among children and adults and symptoms can show up at any age. The infantile-onset type tends to present similarly among infants and within the first year of life.1,3-5
Common Pompe disease symptoms* may include:
- Difficulty breathing, respiratory complications
- Difficulty moving/walking
- Difficulty chewing/jaw fatigue
- Enlarged tongue (macroglossia)
- Muscle weakness
- Low muscle tone (hypotonia)
- Gastrointestinal complications/discomfort such as constipation or diarrhea
- Hearing loss
- Enlarged heart (cardiomegaly, more common in infantile onset form†)
- Developmental delay (more common in infantile onset form)
*These are not all possible symptoms, nor do all individuals have all the listed symptoms.
†Heart involvement in the late-onset type is not as common and when present may involve rhythm problems.
If you suspect Pompe disease, talk to your doctorIf you have any concerns about symptoms or think you or someone in your family might have Pompe disease, talk to your doctor about possible next steps, such as getting tested. |
What causes Pompe disease?
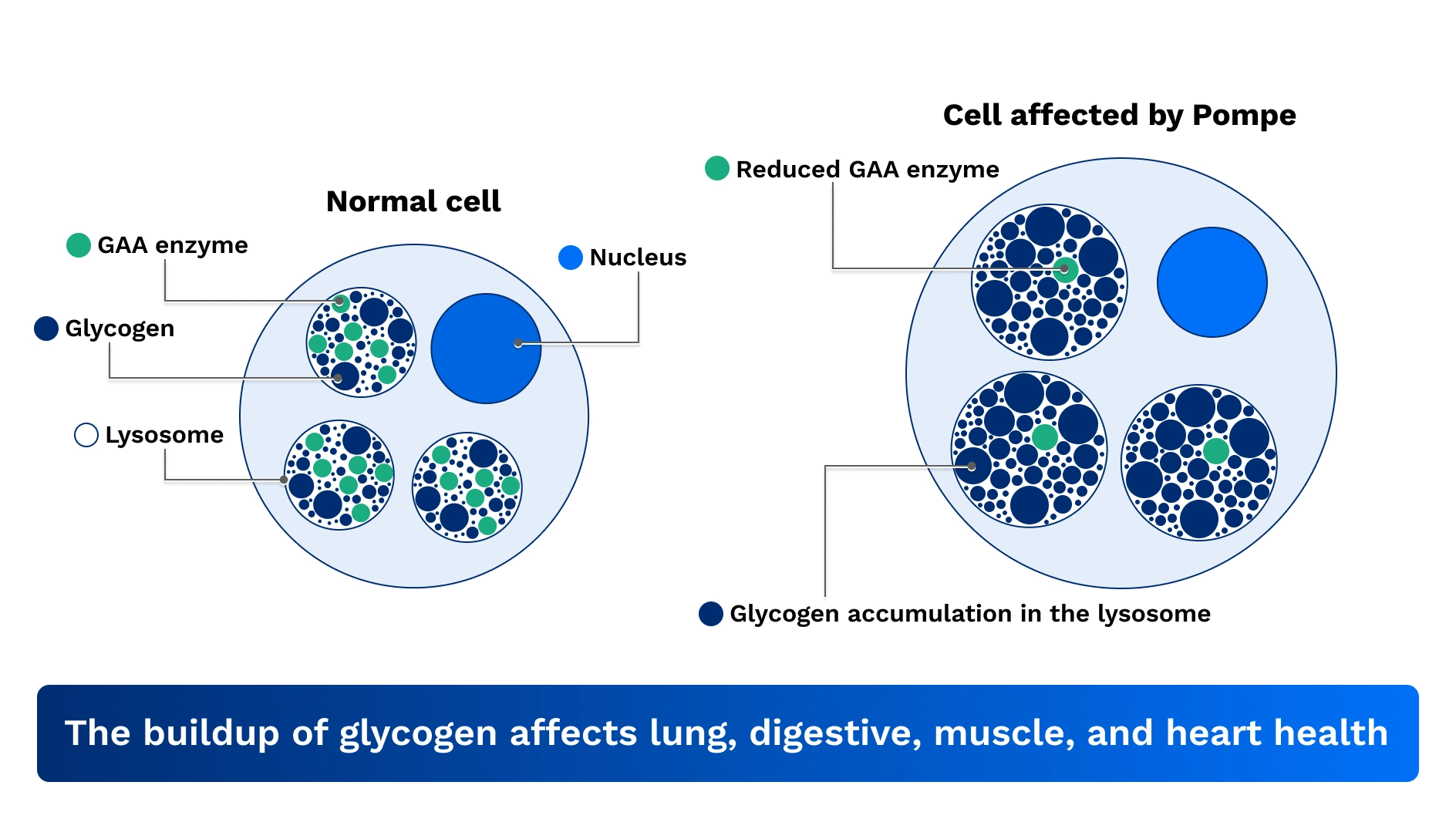
Pompe disease is caused by changes in a gene called GAA. This gene produces an enzyme called acid alpha-glucosidase (al-fuh gloo-koh-si-dey-z), or GAA, which is responsible for breaking down a type of sugar called glycogen.
Alterations in the GAA gene that occur with Pompe disease result in reduced production of the functional GAA enzyme. Without enough working GAA, too much glycogen builds up in the body over time. This buildup can cause muscle weakness and organ dysfunction, leading to signs and symptoms.1
How is Pompe disease inherited?
Pompe disease is an inherited condition caused by alterations (pathogenic variants) in the GAA gene. It has an autosomal recessive inheritance pattern, meaning an individual must have two copies of the altered GAA gene to have the condition. Children inherit two copies of each gene, one from each biological parent. Males and females have an equal chance of inheriting or passing on the altered GAA gene.1,4
A person who has a single copy of the altered GAA gene is called a carrier. Carriers generally do not have Pompe disease or experience symptoms but can still pass on the affected gene to their children.4
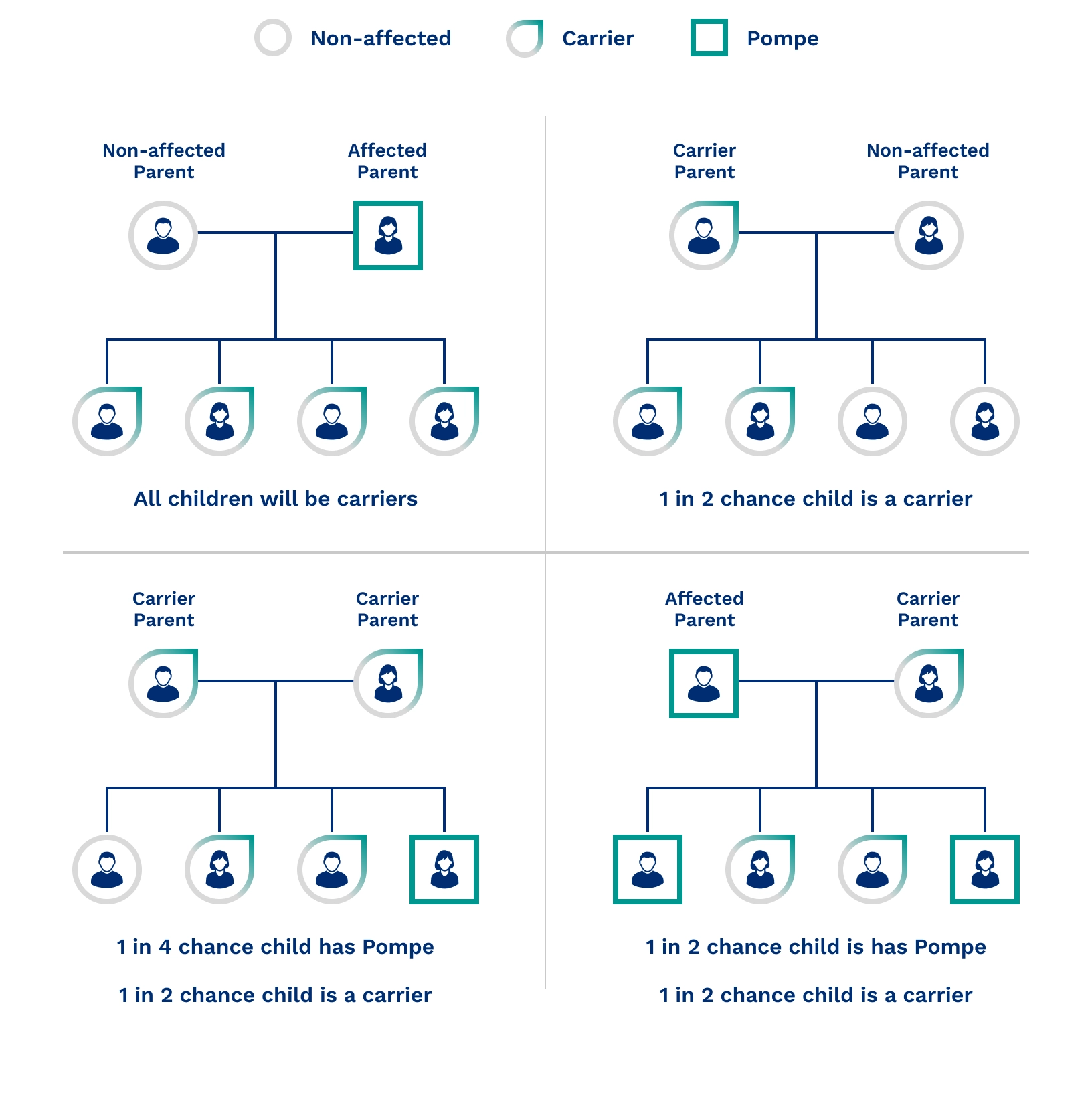
When both parents are carriers, there is:
- A 25% chance that their child will have Pompe disease
- A 25% chance that their child will not have Pompe disease or be a carrier
- A 50% chance that their child will be a carrier of Pompe disease, without having the condition
If one parent has the condition and the other is a carrier, the chance of having a child with Pompe disease increases to 50%. Each pregnancy is an independent event, so the risk remains the same each time.
How is Pompe disease diagnosed?
Diagnostic testing is initiated when a doctor suspects their patient may have Pompe disease based on their family medical history or symptoms.
How to test for Pompe disease:
Enzyme testing
Pompe disease can be diagnosed with a test that measures the activity levels of the GAA enzyme. If decreased GAA activity is seen, this indicates that the individual has Pompe disease. How much the GAA enzyme activity is reduced can vary, especially for individuals with late-onset Pompe disease.
Enzyme testing can be performed using a standard blood sample or skin biopsy, or with a dried blood spot from a heel stick (more commonly used for infants).1,3
Genetic testing
Genetic testing can also be used to confirm a Pompe disease diagnosis and may be preferred by some doctors since it provides a more definitive result. Genetic testing can also determine which pathogenic variants are present. This type of testing may be performed using a cheek swab, saliva, or a blood sample.3,6
Since Pompe disease can be passed down in families, if one family member has the condition, relatives should consider talking with their doctor about getting screened to see if they are a carrier.6
How is Pompe disease managed and monitored?
Monitoring is important for Pompe disease because the condition is progressive, which means it can get worse and symptoms may change over time. Because the condition affects many parts of the body, management plans are often led by a physician who has experience with Pompe disease, such as a metabolic disease specialist or geneticist. A team of specialists is typically involved to properly manage and monitor all symptoms.3,5
Your Pompe disease healthcare team may include:
- Metabolic disease specialist (specializes in conditions involving the body’s metabolism)
- Geneticist (gene specialist)
- Cardiologist (heart specialist)
- Pulmonologist (lung specialist)
- Neurologist (brain and nervous system specialist)
- Neuromuscular specialist (muscle and nerve specialist)
- Physical or occupational therapist (specializes in preserving mobility and function)
Some tests your care team may want to perform include:
- Physical exam: general health and vital signs
- Functional assessments: exercise and muscle strength tests
- Respiratory tests: measure lung capacity and function
- Cardiac scans: monitor heart muscle for thickening
Your primary care doctor or child’s pediatrician can help you communicate with your care team to determine what assessments might be needed and how often, based on your personalized care needs.
Additional resources for Pompe disease
Resources are available to support individuals and their loved ones who may be impacted by Pompe disease. There are patient advocacy groups that support the Pompe disease community, and can help explain the new updates and related findings for people living with Pompe and their caregivers.7 Visit their websites to learn more about them and the services they offer.
This listing is provided for reference only and does not constitute an endorsement by Sanofi of any particular organization or its programming. All other trademarks are the property of their respective owners. Additional resources may be available and should be investigated. Sanofi does not review or control the content of non-Sanofi websites. Additional resources may be available and should be investigated. Sanofi does not review or control the content of non-Sanofi websites.
Acid Maltase Deficiency Association (AMDA)
An organization that promotes public awareness of Pompe disease and collaborates with experts and policymakers with the goal of improving care, ensuring early diagnosis, and supporting affected individuals and their families.
Grant’s Giants
A nonprofit that provides education and advocacy for the Pompe disease community, including support for advancements in research, screening, and helping affected families with medical expenses.
Marshall’s Mountain
An organization dedicated to improving the quality of life of those affected by Pompe disease by fundraising, providing disease education, and offering support and patient advocacy.
Pompe Alliance
A patient-centered organization that provides supportive services, education, and advocacy for people affected by Pompe and their caregivers, engages with medical professionals, and with Pompe disease community stakeholders.
Pompe Warrior Foundation (PWF)
A foundation with the goal of empowering individuals and families affected by Pompe Disease and other lysosomal storage disorders by promoting research and providing education.
Muscular Dystrophy Association (MDA)
A volunteer advocacy organization for people in the United States living with neuromuscular conditions, with the goal of empowering those who are affected to live longer, more independent lives.
Personalized support for people living with Pompe disease
If you or someone close to you is living with Pompe disease and you’re looking for more information about resources or support, contact our CareConnect team Monday through Friday, 8AM-6PM EST.
Call 1-800-745-4447 (for English, press 3; para español, oprima 7) or email info@CareConnectPSS.com.
References
1 Morales A, Siqueira Tavares De Melo MH, Anastasopoulou C, Anilkumar AC. Glycogen Storage Disease Type II. StatPearls. 2025.
2 Lagler FB, Moder A, Rohrbach M, et al. Extent, impact, and predictors of diagnostic delay in Pompe disease: A combined survey approach to unveil the diagnostic odyssey. JIMD Rep. Sep 2019;49(1):89-95. doi:10.1002/jmd2.12062
3 Labella B, Cotti Piccinelli S, Risi B, et al. A Comprehensive Update on Late-Onset Pompe Disease. Biomolecules. Aug 22 2023;13(9)doi:10.3390/biom13091279
4 Sperry E, Leslie N, Berry L, Pena L. Pompe Disease. In: Adam MP, Bick S, Mirzaa GM, Pagon RA, Wallace SE, Amemiya A, eds. GeneReviews((R)). 1993.
5 Kishnani PS, Steiner RD, Bali D, et al. Pompe disease diagnosis and management guideline. Genet Med. May 2006;8(5):267-88. doi:10.1097/01.gim.0000218152.87434.f3
6 Muscular Dystrophy Association. Genetic Testing Options for Pompe Disease. Accessed January 15, 2026. https://www.mda.org/sites/default/files/2022/11/Genetic-Testing-Options-for-Pompe-Disease.pdf.
7 Patterson AM, O'Boyle M, VanNoy GE, Dies KA. Emerging roles and opportunities for rare disease patient advocacy groups. Ther Adv Rare Dis. Jan-Dec 2023;4:26330040231164425. doi:10.1177/26330040231164425
MAT-US-2602117-v1.0-03/2026